Syria’s Health System, On Paper and Off
Syria’s Ministry of Health just published a strategy that names its own failures, scores its own facilities against poverty data, and frames household health spending as a humanitarian emergency.
When liberation came in late 2024, some of the Syrians who had spent the conflict years running health programs from Gaziantep, managing policy from San Diego, watching the system fragment from across a border they could not cross, chose to return. They are now in senior roles inside the Ministry of Health, navigating a bureaucracy that still runs on paper, betting that the institution can be changed from the inside. That choice is the human fact that underlies the document this essay examines, and it is visible in the document itself: in the candor of its baseline data, the rigor of its prioritization methodology, the refusal to write for donors rather than for implementers.
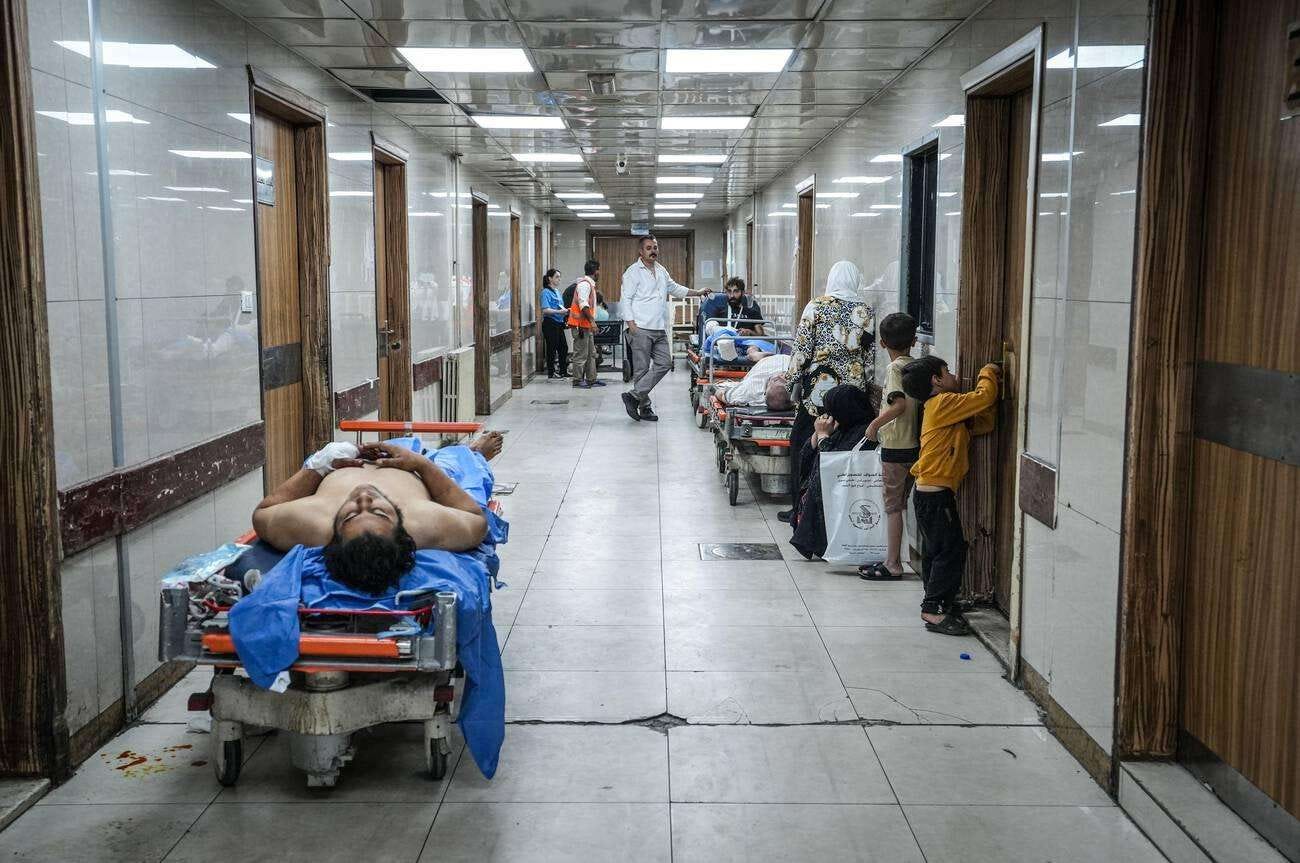
What the sector looks like on the ground is not what the aggregate data alone conveys. The destruction is real and visible, but it is the quieter degradation alongside it that defines the experience of health care in Syria today. Private hospitals operate well below the standard of their counterparts in Amman or Beirut, and the public system did not collapse entirely but contracted over fourteen years into something far smaller than the country requires and far weaker than its regional peers. Syria’s private health sector is frequently cited as the functional backstop when the public system fails; what that framing omits is that the private sector here is itself less developed, less capitalized, and less capable than the private sectors of Jordan, Lebanon, or Iraq, leaving a country of twenty-three million people with no tier of health care operating anywhere near its necessary capacity.
Governments emerging from prolonged conflict tend to produce one of two kinds of planning documents. The first is the vanity document: thick with vision statements, thin on baseline data, written for donors rather than implementers, and quietly shelved within eighteen months. The second is the emergency patch: a triage list dressed as a strategy, reactive by design, institutionally incapable of looking more than one budget cycle ahead. Both are, in their way, a form of institutional self-protection, the appearance of planning without the exposure that comes from committing to something specific enough to fail at.
The Syrian Ministry of Health’s Strategic Plan for 2026 to 2028, published in early 2026 and available in English on the Ministry’s own website, is neither of these things. It names the damage without softening it, publishes the numbers that make the government look bad alongside the numbers that might attract investment, and sets targets specific enough to be held to. It frames the period not as a plan for transformation but as what it actually is: an early recovery phase, a bridge, a foundation for something larger that has not yet been designed.
WHAT THE NUMBERS SAY
As of early 2025, only 54% of Syria’s hospitals were operating at full capacity, and for primary care centers the figure was 39%. More than 90% of medical devices had exceeded five years of operational life. Physician density stood at 2.2 per 10,000 population, against a WHO minimum threshold of 23 combined health workers per 10,000, and approximately half of Syria’s health cadres emigrated during the conflict. The plan cites this figure plainly, from its own sources, without qualification.
On financing, the picture is starker. Government health expenditure in 2022 was approximately 1.41% of GDP, lower than Jordan at 2.49%, lower than Lebanon at 1.96%, and lower than Iraq at 2.18%. Out-of-pocket spending represents 46% of total health expenditure, and in a country where more than 90% of the population lives below the poverty line, that is not a financing inefficiency. It is a mechanism for producing catastrophic health expenditure at scale, the kind that pushes families deeper into poverty at the moment they are most vulnerable.
The plan describes out-of-pocket spending as a humanitarian exposure, which is a political choice as much as a technical one. It signals that the Ministry intends to treat health financing as a social protection question, not merely a budget line, and that signal is there, in print, in a government strategy document. That distinguishes this plan from most of what preceded it.
THE ALLOCATION PROBLEM
The standard critique of post-conflict health strategies is that they are designed to be unfalsifiable. Targets are set vaguely enough that any outcome can be described as progress, baselines are absent or unreliable, and the institutions responsible for monitoring are the same ones responsible for delivery. The MoH plan is not immune to these pressures. Its monitoring framework acknowledges, with unusual candor, that routine data collection across Syrian health facilities is too fragmented to support reliable measurement. The eight strategic pillars, covering infrastructure rehabilitation, workforce development, health financing, service delivery, governance, medicines access, digital transformation, and health security, are ambitious in aggregate and appropriately modest in their 2028 commitments. The plan is not promising to fix the sector by 2028; it is promising to build the tools that would allow the sector to be fixed between 2029 and 2033.
What makes it serious is a specific design choice in the infrastructure rehabilitation pillar: the facility prioritization matrix. When 60% of Syria’s health facilities have structural damage and available capital is a fraction of what rehabilitation would require, the allocation question is politically explosive, and the forces that typically answer it are proximity to the capital, constituency pressure, donor preference, and visibility, producing the predictable distortions of urban bias and the rehabilitation of facilities that photograph well over those that serve populations most in need. The Ministry built a scoring matrix instead, weighting population catchment size, availability of existing health cadres, travel time to the nearest functional facility, poverty rates, and displacement absorption, meaning the degree to which a community is receiving internally displaced persons without corresponding infrastructure, to produce a ranked list that no single political consideration can easily override.
“We could not answer that question with instinct. We needed a framework.” Dr. Salaheddin Safadi, Head of Strategy, Ministry of Health, March 2026
The matrix is imperfect and the underlying data is uneven, but it produces what the plan calls “a defensible allocation logic,” meaning the Ministry can explain, to any external observer and to itself, why it is investing here rather than there. That accountability to method, rather than to political convenience, is what distinguishes planning from performance.
EVIDENCE ABOUT AN INSTITUTION
There is a reading of this document that treats it as evidence about a plan. There is a more important reading that treats it as evidence about an institution. Syria’s post-liberation government inherited a public administration built for a different era and three separate health architectures that had developed independently during fourteen years of war: the Damascus-centered government network, the NGO-sustained northwest, and a distinct system in the northeast, each with its own institutions, funding logic, and embedded habits that did not dissolve when liberation came.
The Ministry was not guaranteed to produce a planning document of this quality. It could have cited data selectively, or written for donors rather than implementers. The fact that it did neither is evidence, not proof but evidence, that the institution has the analytical capacity and political will to work honestly with the problem it has actually inherited. Early institutional output is predictive. A Ministry that in its first major planning exercise builds a weighted scoring matrix and publicly acknowledges that its monitoring data is unreliable is demonstrating the preference for honesty over comfort that is the prerequisite for every reform that follows.
WHAT THE PLAN CANNOT DO
The plan’s most significant constraint is one that candor about baselines cannot resolve and a weighted scoring matrix cannot fund: the gap between what the strategy commits to and what Syria’s fiscal environment can support. Government health expenditure at 1.41% of GDP cannot sustain the rehabilitation, workforce development, and digital transformation the eight pillars describe. The Ministry’s stated goal is to reduce dependence on NGO financing, not to eliminate external funding but to shift its character from project-based humanitarian assistance toward aligned development investment. That is the right objective, but it depends on a level of donor coordination that Syria’s international partners have not consistently delivered, and that the plan cannot compel.
The workforce problem is similarly structural. Emigration of half the health workforce over fourteen years produces gaps in anesthesiology, nephrology, intensive care nursing, and surgical subspecialties that cannot be closed by retention packages in a two-year window. A national workforce census and an HRH roadmap are the correct first steps; what the plan cannot do is compress training pipelines measured in years into the political urgency of the moment. These are not criticisms. They are descriptions of the environment in which the plan must be executed.
THE TEST IS NOT 2028
The most honest line in the document frames the period as “a focused effort to rebuild the foundations of the health system and create the conditions necessary for sustainable development.” By end of 2028, the Ministry commits to a national facility registry, a verified health workforce census, national health accounts, a costed and piloted Essential Health Services Package, and a functioning digital health governance unit. These are not transformation targets; they are the data infrastructure without which transformation cannot be planned.
The test of this strategy is therefore not what Syria’s health system looks like in 2028. It is whether the facility registry gets built in 2026, whether the national health accounts are published in 2027, and whether the Essential Health Services Package is piloted in enough facilities across enough governorates to generate real operational learning before it is scaled. If those things happen, Syria enters the 2029–2033 national health strategy with a genuine evidence base. If they do not, this plan joins the long shelf of post-conflict strategies that diagnosed the problem accurately and then failed at the first level of implementation.
The Ministry of Health has produced a document that deserves to be taken seriously.